
A treatment involving the injection of a local anesthetic next to a bundle of nerves in the neck has eased post-traumatic stress symptoms in some patients in as little as 30 minutes with dramatic, lasting results.
Now, the Pentagon is funding a study at three Army medical centers to determine if the technique — long used for the treatment of pain — is truly effective in treating PTSD.
The results from the largest random, controlled trial using the stellate ganglion block could revolutionize the way PTSD — considered a mental illness — is viewed and treated, according to doctors familiar with the experimental procedure.
“It really is the tipping point,” Col. James Lynch, command surgeon for U.S. Special Operations Command Africa in Stuttgart, who has seen firsthand the promising effects of the shot, said about the current trial.
“It has the potential to be a huge game changer for many, many affected people with PTSD,” whether from combat, sexual assault or other trauma, he said. “There’s really not been a great answer for this giant population.”
The U.S. government has spent millions treating PTSD and searching for effective therapies since the wars in Iraq and Afghanistan thrust the disorder into the national spotlight.
If proved to be effective, the block could provide relief to millions of servicemembers and veterans who suffer from combat-related PTSD.
The stellate ganglion block is offered as treatment for PTSD at a handful of Army hospitals, including Landstuhl Regional Medical Center in Germany, but it has yet to gain wide acceptance as a therapy for the disorder because of the lack of clinical evidence proving the intervention works.
The Pentagon study could change that.
RTI International, a research institute in Raleigh, N.C., received a $2 million grant from the U.S. Defense Department to conduct the trial.
Besides Landstuhl, Womack Army Medical Center at Fort Bragg, N.C., and Tripler Army Medical Center in Honolulu, Hawaii, are participating.
PTSD can occur after experiencing or witnessing a life-threatening trauma and may cause hypervigilance, hyperarousal, flashbacks, fear, anxiety, avoidance, sadness or other symptoms, according to the American Psychiatric Association.
The illness has been particularly vexing for the U.S. military. Diagnosis of the disorder is at an all-time high among servicemembers and veterans, yet the effectiveness of approved treatments, such as drugs and cognitive therapy, has been mixed.

Dr. Richard Erff, chief of the Carl R. Darnall Army Medical Center Pain Clinic, administers cervical epidural steroid injections to a Soldier who suffers from chronic neck and back injuries stemming from his deployment to Iraq.U.S. Army photo by Patricia Deal.
Up to 20 percent of veterans who fought in Afghanistan or Iraq are diagnosed with PTSD in any given year, compared with 12 percent who served in the Gulf War and 15 percent in Vietnam, according to the U.S. Department of Veterans Affairs.
Though millions of dollars have been sunk into research for alternative therapies for PTSD, from virtual reality to cannabis, the stellate ganglion block holds particular promise and should be a high priority for research, according to scientists from Johns Hopkins University. “The rapid response and destigmatization the procedure offers may enable this technique to be beneficial for particularly difficult-to-treat patient populations, including military servicemembers and veterans,” the researchers said in a report published in October in World Institute of Pain.
Recruiting volunteers
Anecdotal evidence indicates that “for a significant portion of patients, relief is near immediate, and that’s very powerful,” said Kristine Rae Olmsted, a behavioral epidemiologist at RTI and co-investigator in the Pentagon-funded study.
But the procedure isn’t proposed as a cure-all, even if it’s proved to be effective, she said. “We still want people to engage with behavioral health providers, to deal with the other psychosocial impacts of PTSD.”
Enrollment for the study began about five months ago. Researchers are hoping to get at least 240 active-duty military volunteers by the time the study concludes in November 2017, she said.
But so far, recruitment of volunteers has been difficult, Rae Olmsted said. The study is open to active-duty servicemembers who have been diagnosed with PTSD or think they might have PTSD. In an effort to increase enrollment, the study was recently opened to servicemembers being treated for psychological or behavioral health issues, LRMC officials said. Volunteers can receive up to $115 for the time they spend participating in the study.
Related: 8 Common Myths About PTSD Debunked »
“The stigma associated with PTSD certainly is a consideration,” Rae Olmsted said of the challenges in recruiting volunteers for the study. Also, “people are a little leery about getting an injection in the neck. For some people, it’s not that big of a deal; for others, it’s quite off-putting.”
Individuals will be screened for PTSD symptoms in advance. The source of PTSD can be any traumatic experience, not just combat, Rae Olmsted said.
Volunteers receive two injections, two weeks apart. One in three receive a placebo of saline solution instead of the active treatment, she said.
There are always risks involved with any injections, said Dr. Jeffrey Tiede, anesthesiologist and the director of LRMC’s Interdisciplinary Pain Management Center, such as bleeding or nerve damage, but with this procedure, “it’s very low risk” and carries a potentially very high benefit.
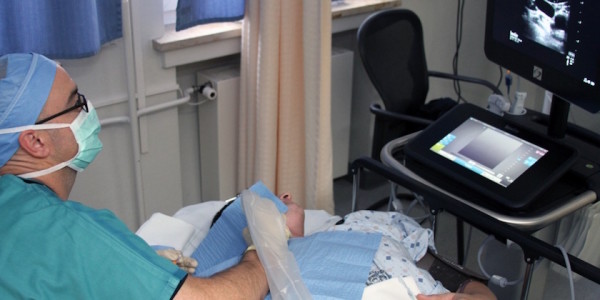
Tiede has administered about 100 stellate ganglion blocks at LRMC this year, mainly for PTSD but for other pain indications, as well, he said. An ultrasound machine is used to help guide needle placement, Tiede said.
“Start to finish, is 10, 15 minutes tops,” he said.
“Even some of the soldiers that are absolutely scared of needles, that have a needle phobia … when they get done, (they say) ‘ah, that wasn’t a big deal at all,’” Tiede said.
From hot flashes to PTSD
The stellate ganglion is a cluster of nerves at the front of the neck. The block is a standard procedure that’s been used for decades to treat chronic pain, Rae Olmsted said.
Chicago anesthesiologist Dr. Eugene Lipov pioneered the procedure for PTSD about 10 years ago, after discovering the block gave relief to women suffering from menopausal hot flashes.
To defend the unorthodox treatment of hot flashes and to better understand why the block was effective, Lipov said he began to research “everything and anything that’s unique” about the stellate ganglion. That’s when he found a Finnish paper on the use of the stellate block to treat anxiety.
Lipov called his brother, Sergei, an internist, and told him: “If you have a patient suffering from PTSD, send him to me.”
Among Lipov’s first patients were Iraq and Afghanistan war veterans with severe PTSD. One was a soldier who had attempted to strangle his wife in his sleep. The shot took immediate effect, but a second block was needed after a fireworks display retriggered some of his symptoms. “He is doing great,” Lipov said.
He believes the block reduces nerve growth factor — a protein necessary for nerve cell survival and new nerve growth — to pre-trauma levels. NGF can surge in response to stress and fear, causing new sympathetic nerve endings to sprout in the brain, Lipov said.
The excess nerves produce more norepinephrine, which is similar to adrenaline, and can trigger chronic stress, heightening the “fight or flight” response, he said.
With the injection, “the whole cascade reverses,” Lipov said, an event demonstrated during experiments on rats. “The sprouting falls off, norepinephrine falls to normal levels and people now are calm and collected.”
Why this happens so quickly is a question that needs further study, he said. He believes it has something to do with the secretion of norepinephrine, which is regulated by the stellate ganglion.
“It takes about 15 minutes for norepinephrine to be removed by the system,” he said. “That is why they feel better right away, I believe.”
Lipov says if the block works, its effects are noticeable almost immediately.
Before administering the injection, he asks patients to think about what caused the trauma. “Women usually cry and men get pissed off,” he said.
After 30 minutes or so, Lipov asks the same question.
“One of the soldiers had a great description,” he said. “He said before the block, he could feel, smell the gore. After the block, he said it feels like he was watching a black-and-white movie.”
Lipov’s initial success rate with the block was about 70 to 75 percent, he said. He’s since pushed that above 90 percent by doing a sequential block. After the first injection, Lipov waits about an hour. If they’ve shown no improvement, he’ll do another injection, higher up in the neck.
“I’ve had almost no failures with this combination,” he said.
The ‘God block’
Lipov had tried for years to get the Defense Department to support a clinical trial on the treatment. Multiple applications for federal funds to sponsor further study had been denied, he said.
The reason the Pentagon finally opened its purse strings was demand from the special operations community, he said.
“The special ops people, they call it the ‘God block,’ because it changes their life and they’re more effective doing their work,” Lipov said.
Lynch, of SOCOM Africa, said he’s never heard it called that, but would agree that use of the block in the special operations community helped push the procedure along. That work began with Col. Sean Mulvaney, currently a pain and sports medicine physician at Fort Belvoir Hospital in Virginia, Lynch said.
As an army special operations doctor, Mulvaney “was getting guys with PTSD that were not coming forward openly and he didn’t have any good answers for them,” Lynch said. “Sean just started googling crazy options” and found Lipov.
Mulvaney set up some of his patients to get a stellate ganglion block at Walter Reed National Medical Military Center by pain providers with experience using the procedure, though not for PTSD symptoms, Lynch said.
“They had dramatic results,” he said.
Lynch admits he was skeptical.
“I couldn’t rationalize the path of physiology in my head,” he said. “I just wrote it off as ‘Sean’s kind of kooky’ and was onto something really kooky.”
Mulvaney and Lynch eventually became certified to administer the block to their patients in special operations units to which they were assigned in the U.S.
They collaborated on several studies and among their findings in the largest case series published: Of 166 military members with multiple combat deployments who received the block, more than 70 percent reported significant improvements in PTSD symptoms three to six months out, according to one study.
Curiously, the block appears to reset the fight-or-flight response, rather than subdue it, doctors familiar with the procedure say.
Lynch said he’s heard soldiers ask: “’Well, hang on a second, you’re telling me you’re going to block my fight-or-flight mechanism? I’ve been training 20 years in the Army to hone that sucker. I don’t want something blocking,’” that, he said.
Lynch and his colleagues did a small study examining reaction time immediately after receiving the block and a week after treatment to make sure there wasn’t a decline in a soldier’s ability to fight.
The outcome “was surprising,” he said. “Things got better. Reaction time got better.”
Though the block has been given to more than 1,000 patients at five U.S. military hospitals and has been studied for years, it’s still not widely accepted as a standard method of care for PTSD, Lynch said.
“Many folks are slow to adopt a new treatment, particularly something that could be invasive, like a needle in the neck, unless there’s adequate literature to show that it’s effective,” he said.
More research needed
Not all studies done on the treatment to date have shown it to be effective, however.
Results published in 2015 from a randomized, controlled trial involving 42 patients at Naval Medical Center San Diego found that stellate ganglion block performed no better than a placebo in relieving PTSD symptoms.
Dr. Robert McLay, a psychiatrist and senior author of the study, said that while the study did not support the use of stellate ganglion block for PTSD, “it also did not eliminate it as a possibility.”
Of the 42 servicemembers with PTSD, 27 were chosen randomly to receive stellate ganglion block and 15 were given a sham injection. Results showed PTSD symptoms improved significantly for both groups after treatment, but there was no clinically significant difference in outcomes between the active and control groups, according to the study. Those who received a second block showed greater improvements, the research team reported.
The study showed definitively that the block “is not a panacea that works for everyone, that there can be a placebo effect from the treatment, and that the procedure, although relatively safe, is not entirely without risks,” McLay told Stars and Stripes in an email.
All medical procedures carry risks, McLay said. With the stellate block, people often will experience a temporary numbing in the arm and face, possibly difficulty swallowing, and there is a small risk of damage to nerves, blood vessels or the lungs, he said.
Lipov questioned the design of the study, pointing to the very small population size involved and that the study did not use an active placebo, one that mimics the side effects of the actual block.
McLay said more research is needed.
“It is definitely worth keeping an open mind,” McLay said. “An open mind doesn’t mean letting your brain fall out, however. We need good science, and that means multiple studies, to support or refute SGB.”
‘It’s like a miracle’
For Brooke Byers, the procedure seemed more miracle than science when she considers the effect it had on her husband, Clint Byers, a former Army intelligence officer, and their family.
About five years ago, Clint Byers returned from a combat deployment to Afghanistan a changed man, she said.
Officially diagnosed with PTSD, he experienced a progressive deterioration in his quality of life. There was memory loss, irritability, insomnia.
“We couldn’t eat out, we could not go to a shopping mall, we could not be in large crowds,” she said. “He was on constant alert and in constant fear. He was constantly scanning crowds and looking for threats.”
Therapy and prescription Zoloft didn’t work, she said.
“He was in bad shape for a really long time,” she said. “It was to the point where I was questioning how much longer I could be in this marriage; how much longer are we going to put the kids through this kind of life that we had at the time?”
Then, Clint Byers’ father saw Lipov on TV talking about the stellate ganglion block on “The Doctors.”
The Byerses scraped together $1,000 to cover the procedure — the VA wouldn’t pay for it — and airfare for the couple to fly from their home in Tampa, Fla., to Chicago, where Lipov practices.
Clint Byers received the block in May 2015. The effects took hold almost immediately.
“He was giddy. He was just so happy and joyful for the first time in several years,” Brooke Byers said.
Those feelings persisted into the next day.
“He literally leapt out of the hotel bed and flung the curtains open, he was so elated,” she said.
On the plane trip home, Brooke Byers turned to her husband and said: “’I’m so happy that you’re so happy, but I’m going to need you to dial it back a bit,’” she said, laughing at the memory. “I told him everybody on the plane doesn’t need to hear how happy you are. I thought, ‘Oh, Lord, they’re going to think he’s on something.’”
She said she was on high alert for several weeks after the procedure. “I was so paranoid it was going to wear off all of a sudden, because we don’t know how long it will last,” she said.
“He’s still great,” she said. “I’ve got this man back whom I have not known in years. It’s like a miracle, no joke.”
Lynch urges those who have or think they may have PTSD to at least consider participating in the current study.
He’s heard soldiers express concern about not wanting to be a “guinea pig” by participating in an “experimental” study. The study, he emphasized, is not experimental; the procedure has been performed for a number of years and numerous studies have been done, just none large enough to propel the treatment into the mainstream.
“It will take having enough participants in this study to truly determine whether SGB is effective,” Rae Olmsted said. “If it is, then the procedure can be adopted tri-service-wide, as well as in veteran and civilian communities, to offer hope to those suffering from the often debilitating symptoms of PTSD.”
———
© 2016 the Stars and Stripes. Distributed by Tribune Content Agency, LLC.