For rural veteran Mickey Ireson, appointments at the Department of Veterans Affairs are a source of apprehension and stress, rather than relief. In early April, the former Marine infantryman received a call from the VA telling him that his evaluations for mental health and dental work had been scheduled at the Omaha, Nebraska, office.
Ireson lives three hours away in Hastings.
Initially scheduled for three separate days, Ireson was able to have the appointments moved to one day, but that meant six hours worth of driving, and several hours of meetings with physicians and caregivers. For Ireson, who is employed and going to college on the Post-9/11 G.I. Bill, lengthy travel time can mean a day behind in class, or a day’s worth of wages lost. In addition, Ireson has trouble being on the road for several hours at a time, and the frustration that comes with hunting for parking in a crowded lot, and long wait times once he arrives, only makes him more agitated and apprehensive about the VA.
“Driving to Omaha doesn’t make it any easier,” says an exasperated Ireson, who left for his appointment at 5 a.m, and didn’t return home until after 3 p.m. “That’s one more thing to stress out about, there goes a whole day of class, now I have to make up for class, there goes money I was making, there goes fuel I was spending. I don’t know any civilian that drives three hours for a doctor’s appointment.”

Veterans from rural America, like Ireson, consistently shoulder a disproportionate portion of the national security burden, yet they face more obstacles in seeking health care services through the VA than their urban counterparts. Although the challenges facing rural veterans may be caused more by geography than a lack of policy reform, so long as rural veterans are limited in their access to care, they will remain underserved.
Rural America is vital to our nation’s military, and therefore, its security. Rural Americans account for just 20% of the population, but provided 44% of America’s military recruits in 2010, according to research published in the Journal of the Catholic Health Association of the United States in 2013.
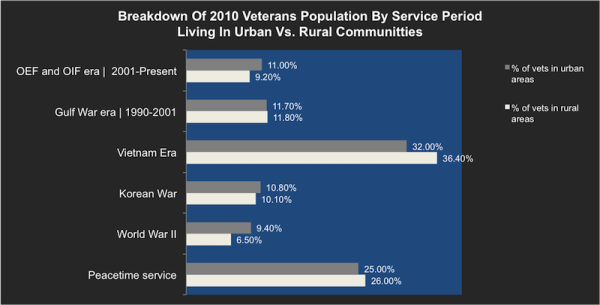
This tradition of service is evident in the roughly two million rural Americans who served after September 11, 2001, and previous generations of veterans who fought in Vietnam, Korea, and during World War II. Of the nine million veterans enrolled in the VA health care system, approximately 3.2 million, or 35%, are living in rural or highly rural areas, according to a fact sheet provided by the VA’s Office of Rural Health. However, according to figures provided to Task & Purpose by the Office of Rural Health, states like Vermont have much higher rates of enrolled rural vets, with 88% of its total veteran population, or 21,000 people, living in small towns as of 2014. Comparatively, Texas has the highest number of registered rural vets — 212,000 — but this figure only represents 30% of its enrolled veteran population.
For many growing up in rural America, military service can mean professional training and work experience that might be transferable in the private sector, and the Post-9/11 G.I. Bill provides a college education, paid in full, which offers a means for upward economic mobility. Of course, there’s also the drive to serve, especially in a region where it’s not uncommon, but is in fact more akin to the status quo. According to the Office of Rural Health website, youth from rural America are 22% more likely to join the Army than those from urban areas. While joining the military can offer a host of opportunities for young men and women, returning to those rural communities after completing their service can create an equal amount of hardship.
Transitioning out of the military can be exacerbated by living in a rural area for post-9/11 veterans like Ireson. When he left active duty in 2012, he did what many service members do; he moved off base. Ireson had served with 2nd Battalion, 2nd Marine Regiment, and deployed twice, first to Afghanistan, and then with the 22nd Marine Expeditionary Unit. Growing up in the foster care system in California and Florida, Ireson couldn’t afford to move to his mother’s home in Nebraska, so he decided to stay near the Marines he served with and ended up living in Wilmington, North Carolina. While there, Ireson found little opportunity to restart his life and even less support. He spiraled downward, and eventually ended up in rural Kansas, homeless, penniless, recovering from substance abuse, and struggling with post-traumatic stress disorder.
For some veterans, including Ireson, seeking treatment through the VA involves navigating a labyrinth of bureaucratic policy, numerous impersonal phone calls, and frustrating encounters with claims officers or care providers. For rural veterans, this process is exacerbated by long distances to the nearest facilities and limited access to those facilities, limited and inadequate choices in providers, and a lack of specialty services. Yet, while rural veterans have the least access to care compared to their peers, they face some of the most complex health care issues. For instance, roughly 36% of veterans with a service-connected disability are from rural areas, according to an Office of Rural Health fact sheet. More generally, the VA reports that rural veterans report lower health-related, quality-of-life scores and face a higher prevalence of physical illness compared to urban veterans.
With rural veterans comprising a significant proportion of enrolled veterans, they need a system designed for them, for their needs — the same one used for urban areas just won’t work there.
That’s where the Office of Rural Health comes in. Established in 2007, its mission is to improve the access and quality of care for enrolled rural and highly rural veterans, and to create programs, employ strategies, and use emerging technologies to increase health care options for all rural veterans.
Task & Purpose reached out to the Office of Rural Health to ask about the problems it faces in caring with the rural veterans community.
“I think the creation of the office acknowledges that there are unique challenges in delivering care into rural areas whether you’re a veteran or not,” says Gina Capra, the office’s director, located in Washington, D.C. “Certainly those challenges can be particularly acute or unique if you are a veteran and have specific needs related, from your time in service.”
Many of the challenges facing rural veterans apply to rural Americans at large, and Capra says that shortages in health and specialty-care providers, hospital access, and geographic barriers are the main obstacles hampering access to care.
Another challenge comes from trying to gather data on rural veterans.
Hilda Heady, a researcher who has studied rural veterans for years, explains why many veterans will not identify themselves as such, especially in rural areas. Rural people are problem solvers, and those who are valued in their community exhibit a resourceful stoicism in the face of adversity.
“If you are a veteran, it’s very normal in a rural community to see service in the military, it’s not special,” says Heady, who is the senior vice president and chair of the rural health policy group, Atlas Research, based in Washington, D.C. This mentality can lead to a resistance to care if it is not readily available.
Heady identifies three barriers facing rural veterans seeking VA health care: access to a care facility, visibility or awareness of the challenges facing rural veterans, and finally, cultural barriers between rural veterans and their care providers.
Much of what is taken for granted in an urban area — easy access to stores, hospitals, public transportation, and highways — is not as commonplace in rural America.
“What I find is, when you start talking particularly about health care access in terms folks can relate to, they tend to get it,” says Capra.
When trying to explain rural challenges to others, Capra explains that it’s like living in a place where you have to drive 45 minutes to a grocery store to get milk, then drive another 45 minutes in the opposite direction to get the kids from school. And if the car breaks down, there may not be any cell phone reception or public transportation.
This anecdote doesn’t even take into account whether or not a person is in need of regular treatment at a clinic or hospital, like a veteran with a combat-related injury in need of routine care.
“When we think about prosthetics and spinal cord injuries, or traumatic brain injuries, these are all often unique to veterans, so we have to think about how distance and time and access to a limited provider workforce has implications,” adds Capra.
These are the real-life challenges facing rural veterans on a daily basis. There might not be an easy solution, and when it comes to distance, there may be no solution at all — policy changes can only go so far; they can’t make a commute any shorter.
Following last year’s VA scandal, Congress quickly passed the 2014 Veterans Access, Choice and Accountability Act, which provided a number of significant reforms aimed at increasing accountability within the VA, providing private care to veterans without easy access to VA facilities, and more.
The bill included $10 billion for the Choice Card Program, which was rolled out last November to help veterans who had been waitlisted for more than 30 days or had to travel more than 40 miles to receive care from a VA facility. The program is meant to allow qualified veterans to receive care from pre-approved private care providers, but it had a rocky launch.
An initial survey conducted by the Veterans of Foreign Wars showed that only 19% of the survey participants qualified for the Choice Card Program perceived being offered the option to use it.
When asked about the Choice Card Program, Ireson said he’d never even heard of it.
The program was also met with confusion and frustration by some veterans and care providers due to the language of the bill, which allowed veterans to receive care if they lived more than “40 miles as the crow flies” from a VA facility. This metric has since been revised to actual driving distance, and will now be calculated using the fastest route rather than the shortest route.
There are concerns that the Choice Card Program doesn’t consider the time it takes to reach a facility. Winding roads, physical barriers, like mountains, bodies of water, or access to a highway, mean that a veteran might end up spending as much time getting to an approved private care provider as he or she would spend getting to a VA clinic. And, there’s always the possibility that a veteran simply lives too far from either a VA facility or private care provider for the program to make a difference.
Policies like the Choice Card Program can’t unwind roads, knock down mountains, or remove bodies of water. This is where the tough question for veterans and the VA start: Where does the government’s responsibility stop, and where does the individual’s responsibility to receive care, begin?
For Ireson, whether or not to seek care from the VA was a matter of finance. Even now that he is enrolled in the VA, and his financial situation has improved, Ireson says he still cannot afford to take time away from work to go to the nearest VA — an hour or more each way — not including the time at the doctor, would mean that many hours worth of wages lost. Ireson, who was diagnosed with PTSD, suffers from anger, dissociation, anxiety, and depression. He was also diagnosed with back, knee, and shoulder problems, and is in the process of seeking VA care for issues with his jaw and missing teeth.
“I need this or that done, and they’re asking me to drive three hours away for an appointment,” says Ireson, referring to dental appointments and consultations to replace his missing teeth. “I’m in class full time, I have a job, the amount of driving involved with it — nobody I know has a lot of money, nobody’s doing good financially. I don’t have time to travel three hours for a five-minute meeting with someone. I can’t do that.”
In addition to tough fiscal choices, veterans leaving military service, especially those with acute injuries or health problems, can be caught between heading home to where their families and friends are or staying near a base or large city where they can have easier access to care. In essence, veterans from rural communities may face sacrificing their support networks for personal health.
Access doesn’t just mean distance between a veteran and a clinic, though that is certainly a problem for many. It can also refer to an individual’s access to transportation, which is a common hurdle for rural veterans. According to research conducted by Heady in 2013, 54% of households have only one car, 5.6% do not own a car at all, 11.15% don’t have a valid driver’s license, another 13% rely on family and friends for transportation, and 11% use van services provided by nonprofit organizations.
Access also refers to how often a clinic or claims office is open during the week, and this can have far-reaching effects on how rural veterans view, interact with, and use — or don’t use — the VA system. In fact, out of 22 million veterans living in the U.S, less than half are registered with the VA.

Limited office hours are common in rural areas, where it may not be feasible to have an office fully staffed 40 hours a week in a small town. Commonplace as it may be, the effect can be devastating when someone comes to a door, only to find it locked. It shatters trust, explains Ryan Kaufman, a 32-year-old Army veteran living in Grand Island, Nebraska.
Kaufman went through this exact situation himself a few years ago, when he went to a claims office at the Merrick County courthouse a few blocks from where he was living at the time, only to find the place closed.
“There was a number on the wall, and my first reaction wasn’t professional. I had some expletives fly out my mouth,” says Kaufman, who decided to call the posted number and give the other end a piece of his mind. Afterward, Kaufman drove to the Hall County veterans service office where they handled his claim.
“Guys like us struggle with trust,” explains Kaufman. “We don’t trust anyone, at all. So I’m going to leave my name and number, and I forget because I don’t think you’ll ever call me back, and that’s been my experience.”
About a year later, while at the American Legion in Central City, Nebraska, Kaufman met the veteran service officer who left the note on the wall of the courthouse and found that he actually makes house calls and can be reached on his personal phone at all hours.
This is not unusual in rural America where a personal connection between members of the community is probably the most reliable way to solve a problem. However, it also demonstrates that while at a national level, the VA has pledged billions of dollars to improve care for veterans, there are still entire communities slipping through the cracks.
That’s where Kaufman, who’s now a peer specialist and program coordinator for the Lutheran Family Services of Nebraska’s At Ease Program, comes in. At Ease provides confidential counseling services for active military personnel, veterans, and their loved ones, regardless of their ability to pay.
“My job is to take them to the case workers that if I had a problem I would go to,” says Kaufman, who uses his list of personal and professional contacts to help veterans in need. “I take them to the resources that if my ends weren’t being met, I would go to.”
Which is what happened when Kaufman met Mickey Ireson in 2014.
“When I got out, I had a hard time mentally,” says Ireson.“I was real bad into drugs from when I was in the Marine Corps, and couldn’t get a job anywhere. Nobody wants to hire veterans off base. I couldn’t even get a job washing dishes at a restaurant.”

When Ireson left the Marines, he had trouble finding work, at one point, he even submitted more than 150 applications in a single month, with nothing to show for it.
“It was pretty rough,” he adds.
Prior to leaving active service, he attempted to enroll in the VA health care system, and had trouble getting the process started, which continued after he separated.
“I tried getting a hold of the VA before I got out, like everybody told me to and I didn’t get anywhere with that. I kept getting, ‘You called the wrong place, call this guy, then call that guy’ and after about 15 phone calls I gave up,” he says.
Ireson’s patience eventually gave out and by that time, he was out of work, out of money, and on drugs with nowhere to go.
And, like the story shared by so many veterans, that might have been the end of it. Ireson could’ve become another tragic and cautionary tale of a military transition gone wrong, hampered by drug use and financial issues. But that wasn’t the case, though his road to recovery would be long and hard.
In April 2013, Ireson attempted to make a fresh start in Kansas, taking his foster brother up on a longstanding offer for work on a farm. When he arrived, there was a job, but no money.
“Had my pickup sold and packed up everything I had, drove up there in a U-Haul and found out the guy was broke, owed money, and was getting arrested every week,” says Ireson, who agreed to stay on in the hopes of future pay.
There was a silver lining, however. During his time on the farm, he kicked his drug habit because he couldn’t afford it.
Ireson stayed at his brother’s farm until November of that year, and then held a string of odd jobs, until he eventually found himself squatting in a dilapidated house. It was at the beginning of August 2014, through Project Homeless Connect, an organization that helps homeless individuals and families, that Ireson met Kaufman.
In the span of 15 days, Kaufman helped Ireson get an apartment in Hastings, Nebraska, with rent taken care of for more than six months. Ireson also received other necessities like pots and pans, food, gas for his pickup truck, cards to get a hold of VA employees and service representatives, and contacts to help with his disability claim, in addition to assistance enrolling in college.
On August 17, Ireson moved to Hastings and the next day, he started school at Central Community College.
The sudden outpouring of support may have quite literally saved Ireson’s life. He is still enrolled in school, is the president of the student veterans club, has a 3.8 GPA, gainful employment, and a stable living situation.
Sometimes ensuring proper care for veterans involves walking a veteran to each person he or she needs to see at the VA, and ensuring that the right paperwork is filed with the right individual, at the right time. Kaufman describes this approach as a continuation of care, from one hand to the next. What makes this unique is that it’s essentially a grassroots solution to big government bureaucracy. For example, in Grand island, Lutheran Family Services of Nebraska and the Iraq and Afghanistan Veterans of America schedule “vet togethers,” where local veterans and their families can gather and network, over food and drinks.
“In this country we get words confused, we have a war on poverty, we have a war on education, a war on drugs — we use that word far too often without people understanding what that looks like, and we use care the same way,” explains Kaufman. “If 22 guys are dying in a VA in Phoenix and nobody knows about it, that’s not care. If we have a backlog of over 400,000 veterans, that’s not care. It seems as though nobody cares. My job is to take them to those community members who do, and usually they’re the ones who have been there and done that.”
Traditional modes of care include VA hospitals and community-based outreach clinics, but it’s not always feasible to establish a physical presence in a rural, or highly rural, area. Another form of traditional care involves the VA working with existing private care providers in local communities.
The VA has also created new programs specifically for veterans in remote areas, like telehealth, which allows a veteran to communicate electronically with a physician. In 2013, more than 600,000 veterans received some element of health care via telehealth, amounting to roughly 11% of veterans enrolled in the VA health care system, according to the VA.
“I think things are getting better, but they do have to get better faster because of the challenges being brought in by the post-9/11 veterans,” Heady says, referring to the additional strain that the VA is finding itself under as this newest generation of veterans grows.
A Department of Defense spokesman, Lt. Commander Nate Christensen, told Task & Purpose via email that roughly 200,000 service members leave the military annually. This means that each year, there are an additional 200,000 men and women who may require health care services through the VA.
The coming years will be critical. It remains unclear whether the VA will be able to meet the growing needs of a new generation of veterans, in addition to the considerable demands already placed on the department.
Perhaps the solution lies with rural veterans like Ireson and Kaufman who turn to local and community-based support, preferring to work with veteran service organizations and peers in order to navigate a system that doesn’t feel tailored to them, or able to meet their specific needs.
As with any other group or demographic with its own culture, background, and shared experiences, veterans can sometimes be best served by those who have borne the same burdens, suffered the same hardships, and overcome the same obstacles.
For Ireson, it appears that the low points in life are the catalysts for self-improvement, and for those struggling to readjust to life outside of the military and a life away from war, it can help to be reminded that others have tried, faltered along the way, and ultimately succeeded.
“If I keep fighting on, and if I do good in life I can turn around and I can show people what I have done,” Ireson says. “I can help them out. I can say ‘I’ve been through this, like you. You can trust me.’ I can show them the way, I’m not just telling them, I can show them because I did it.”

